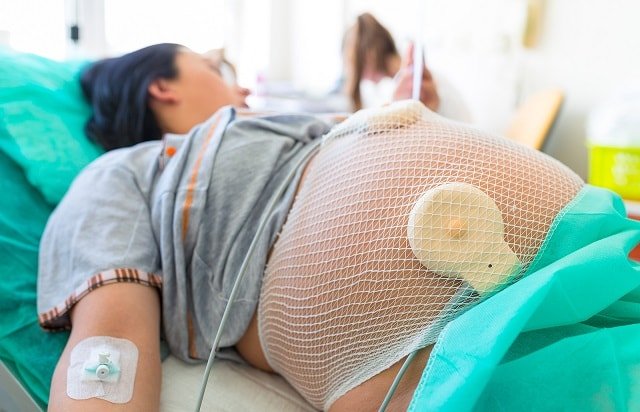
When women become pregnant or try to conceive, they hope to have a normal, smooth-sailing pregnancy and deliver a healthy baby.
Unfortunately, many mothers-to-be develop a high-risk pregnancy, which exposes them to a wide range of complications and even threatens the health and lifespan of their unborn baby.
Different factors can increase the risks that pregnancy brings, although studies show that only six to eight percent of all pregnancies result in high-risk complications.
If your doctor has diagnosed you with a high-risk pregnancy, or if you feel that you might have one, read this guide to know what to expect in the next nine months and beyond.
What Puts a Pregnancy at High Risk?
Before anything else, let’s take a look at what makes a pregnancy have higher risks than others. The following factors can increase your chances of having a risky pregnancy:
Age— If you get pregnant before you turn 17 years old, your pregnancy will be considered high-risk since your body is not yet fully developed to carry a child.[1] If you get pregnant over 35 years old, you have higher risks of developing pregnancy-related health problems (discussed below).
Weight — Being overweight or obese makes you a candidate for a high-risk pregnancy. This comes from the fact that your weight increases your chances of developing high blood pressure, gestational diabetes, preeclampsia, and other conditions that might threaten your pregnancy.
Existing Health Conditions — If you have diabetes, high blood pressure, kidney disease, epilepsy, and other health problems before you get pregnant, your pregnancy will be considered high risk since these conditions make carrying a baby difficult.
This is also the case if you have infections like HIV, gonorrhea, syphilis, hepatitis C, rubella, and chickenpox since the bacteria and viruses involved can harm your baby, and the medications to treat them can be harmful to your baby.
Pregnancy-Related Health Issues — Even if you were healthy before you got pregnant, there’s still a chance that you could develop health problems during your pregnancy.
Some women, for example, don’t have diabetes, but they developed gestational diabetes when they got pregnant. This can still increase the risks they face during pregnancy.
Multiple Births — If carrying a single baby is difficult, it becomes even more so when you’re carrying twins, triplets, or more. Having a multiple-birth pregnancy increases your chances of developing pregnancy-induced diabetes and high blood pressure and experiencing preterm labor.
Substance Use/Abuse — Smoking, drinking, and drug use make it difficult for you to conceive. If you do get pregnant, they’ll make you face a wide range of health risks, particularly if you don’t quit the habit during your pregnancy.[2]
Pregnancy History — If you’ve been pregnant before, and you suffered a miscarriage, preterm labor, preeclampsia, or eclampsia, there’s a chance that you’ll experience these issues again in your current pregnancy.
Medication Use — Certain medications can affect your baby’s growth and development and cause birth defects. They even increase the risk of miscarriage.
Some medications for autoimmune diseases (such as lupus and multiple sclerosis) have been found out to be harmful to the unborn baby. Other medications that are not ideal for pregnant women include phenytoin, carbamazepine, and valproic acid.
The condition of the Baby — The risk to your pregnancy increases if your baby has been found out to have a genetic condition such as Down Syndrome or problems with the heart, kidney, or lungs.
This is also the case if he grows slower than normal or if he’s positioned in a way that doesn’t allow for normal vaginal delivery (e.g. placenta previa, in which the placenta partially or fully covers the cervix).
Signs and Symptoms to Watch Out For
Since high-risk pregnancies can be caused by a wide range of factors, different mothers-to-be should watch out for different signs and symptoms.
But, no matter what factors have made your pregnancy high-risk, you should always be on alert for the following things and call your doctor right away if you experience them:
- Fever
- Severe headache
- Spotting or light bleeding
- Dim or blurry vision (or, if you have existing vision problems, your eyesight has gotten worse than before)
- Swollen face, hands, and/or feet
- Pain or cramping sensation in your abdominal area
- Persistent lower back pain
- A sudden gush of vaginal fluid
- Regular contractions within one hour
- Fewer or zero movements from your baby
If you experience the following signs and symptoms, call 911 right away. They indicate problems that can threaten your baby’s life and yours:
- Heavy vaginal bleeding
- Fainting/losing your consciousness.
- Severe pain in your pelvis or abdominal area.
- The vaginal fluid that is leaking or gushing out, with or without tinges of blood, along with the sensation that the umbilical cord is pushing out into your vagina.
Managing a High-Risk Pregnancy
If your doctor thinks you’re having a high-risk pregnancy, he’ll run several laboratory tests to confirm it. Aside from the basic prenatal physical checkup and blood tests, he might recommend a biophysical profile (which includes fetal ultrasound and heart rate monitoring) to determine the condition of your baby.
If genetic issues are suspected, your physician might advise amniocentesis or chorionic villus sampling (CVS), which can determine if your baby has birth defects.
He might also do a cervical length measurement and do a vaginal swab for fetal fibronectin to find out if you’re at risk for preterm labor.
Of course, you’ll need to follow all the advice of your doctor. For instance, if you have preeclampsia, your doctor might put you on bed rest to prevent your blood pressure from going up.
If this is the case, stay on bed rest as much as possible and make arrangements to have someone else manage your home and take care of your kids and pets if you have them.
Your doctor will most likely recommend delivery in a hospital that has the right facilities to care for high-risk mothers and newborns.
This can be disappointing if you’ve been planning to have a home birth, but your safety and the safety of your baby should come first.
How It Can Affect Your Baby
Just because you have a high-risk pregnancy doesn’t mean that everything won’t turn out all right. Many high-risk pregnant women have given birth to healthy babies, which could also happen in your case.
Even if your baby is born early and needs to stay in the neonatal ICU for some weeks, he can still grow up to become a healthy and happy child.
To make this possible, you’ll need to work closely with your doctor and other healthcare providers to ensure that you and your baby can stay safe throughout the pregnancy.
References