Polycystic Ovary Syndrome (PCOS) is a common hormonal disorder that affects millions of women worldwide. It is characterized by a range of symptoms, including irregular menstrual cycles, ovarian cysts, and hormonal imbalances. Many women with PCOS experience menstrual irregularities, which can have a significant impact on their overall health and quality of life. In this article, we will explore how PCOS impacts menstrual health and provide insights and solutions for managing this condition.
One of the most common symptoms of PCOS is irregular menstrual cycles. Women with PCOS may experience infrequent periods, heavy bleeding, or prolonged periods. These menstrual irregularities can make it difficult to predict ovulation, which can affect fertility. In addition, irregular periods can lead to other health problems, such as endometrial hyperplasia, a condition in which the lining of the uterus becomes too thick.
PCOS can also cause hormonal imbalances that affect menstrual health. Women with PCOS often have higher levels of androgens, such as testosterone, which can interfere with the normal functioning of the ovaries. This can lead to anovulation, a condition in which the ovaries do not release an egg each month. Anovulation can cause infertility and other health problems, such as ovarian cysts. In the following sections, we will explore how to manage menstrual irregularities and hormonal imbalances associated with PCOS.
Understanding PCOS
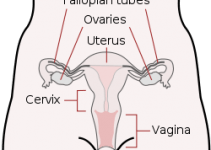
Polycystic ovary syndrome (PCOS) is a hormonal disorder that affects women of reproductive age. It is the most common endocrine disorder in women, affecting approximately 10% of women worldwide. PCOS is characterized by an imbalance of hormones, including androgens, which are male sex hormones that are also present in women in small amounts.
Women with PCOS may have enlarged ovaries with small cysts, which can lead to irregular menstrual cycles, infertility, and other health problems. In addition to menstrual irregularities, common symptoms of PCOS include hirsutism (excessive hair growth), acne, and weight gain.
The exact cause of PCOS is not fully understood, but it is thought to be related to insulin resistance and hormonal imbalances. Insulin resistance can lead to high levels of insulin in the body, which can cause the ovaries to produce more androgens. This can lead to a vicious cycle of androgen excess, insulin resistance, and further hormonal imbalances.
Diagnosis of PCOS is typically based on a combination of symptoms, physical exam, and blood tests to measure androgen levels. Treatment options for PCOS may include lifestyle changes, such as weight loss and exercise, as well as medications to regulate menstrual cycles and reduce androgen levels.
PCOS and Menstrual Health

Polycystic Ovary Syndrome (PCOS) is a hormonal disorder that affects many women of reproductive age. One of the most common symptoms of PCOS is menstrual irregularity. Women with PCOS often experience missed or irregular menstrual periods, which can lead to difficulty in predicting ovulation and making it harder to conceive.
Menstrual irregularity can also cause other menstrual symptoms, such as severe menstrual cramps, heavy bleeding, and prolonged periods. These symptoms can be debilitating and interfere with daily life. It is important to seek medical attention if you experience any menstrual irregularity or severe menstrual symptoms.
Women with PCOS may have a longer menstrual cycle than average, with periods occurring every 35 days or more. This is because PCOS disrupts the normal hormonal balance that regulates the menstrual cycle. Women with PCOS may also have elevated levels of androgens, which can cause acne, excess hair growth, and other symptoms.
There are several solutions available to help manage menstrual irregularity in women with PCOS. Hormonal birth control is a common treatment option that can help regulate the menstrual cycle and reduce symptoms. Metformin, a medication used to treat diabetes, can also be effective in regulating menstrual cycles in women with PCOS.
In addition to medication, lifestyle changes can also help manage menstrual irregularity in women with PCOS. Eating a healthy diet, exercising regularly, and maintaining a healthy weight can help regulate the menstrual cycle and reduce symptoms.
Overall, it is important to seek medical attention if you experience any menstrual irregularity or severe menstrual symptoms. With the right treatment and lifestyle changes, women with PCOS can manage their menstrual health and improve their overall quality of life.
Complications of PCOS
Polycystic Ovary Syndrome (PCOS) is a complex endocrine disorder that affects women of reproductive age. While the exact cause of PCOS is unknown, it is characterized by hormonal imbalances that can cause a range of complications. In this section, we will discuss the various complications of PCOS.
Reproductive Complications
One of the most common complications of PCOS is reproductive issues. Women with PCOS may experience irregular menstrual cycles, anovulation (lack of ovulation), and infertility. PCOS is the most common cause of infertility in women of reproductive age. According to a study, primary infertility was reported in 50% of women affected by PCOS.
PCOS can also cause an increased risk of miscarriage and gestational diabetes during pregnancy. Women with PCOS may also have an increased risk of endometrial cancer due to the hormonal imbalances that occur with the disorder.
Metabolic Complications
PCOS is also associated with metabolic complications. Women with PCOS are at an increased risk of developing insulin resistance, which can lead to type 2 diabetes. Insulin resistance occurs when the body’s cells become resistant to the effects of insulin, which is a hormone that regulates blood sugar levels.
Women with PCOS may also have high levels of androgens, which are male hormones that can cause hirsutism (excessive hair growth), acne, and oily skin. Androgens can also cause metabolic complications such as high cholesterol and high blood pressure.
Psychological Complications
PCOS can also have psychological complications. Women with PCOS may experience depression, anxiety, and decreased quality of life. PCOS can also cause body image issues due to the physical symptoms such as hirsutism and acne.
Diagnosing PCOS
When it comes to diagnosing PCOS, there is no single test that can confirm the diagnosis. Instead, we rely on a combination of medical history, physical exam, blood tests, and ultrasound to make a diagnosis.
To start, your healthcare provider will discuss your medical history and any symptoms you may be experiencing. This can include irregular periods, acne, excess hair growth, and weight gain. They will also ask about any medications you are taking and any medical conditions you may have.
Next, they may perform a physical exam to look for any physical signs of PCOS, such as excess hair growth or acne. They may also perform a pelvic exam to check for any abnormalities in the ovaries.
Blood tests can also be helpful in diagnosing PCOS. They may test your hormone levels, including testosterone, LH, FSH, and insulin. These tests can help us determine if your hormone levels are abnormal, which can be a sign of PCOS.
Finally, they may perform an ultrasound to look for any cysts on the ovaries. While not all women with PCOS have cysts, the presence of cysts can be a sign of the condition.
Overall, diagnosing PCOS can be a complex process that requires a combination of medical history, physical exam, blood tests, and ultrasound. If you are experiencing symptoms of PCOS, it is important to speak with your healthcare provider to determine the best course of action.
The Different Types of PCOS
PCOS is a complex hormonal disorder that affects many women worldwide. It is caused by imbalances in the levels of hormones such as insulin, androgen, and estrogen. There are different types of PCOS, and each has its unique set of symptoms and causes.
The first type of PCOS is the insulin-resistant type. This type is characterized by high levels of insulin in the body, which can lead to weight gain, acne, and irregular periods. Women with this type of PCOS often have a difficult time losing weight, and they may also be at a higher risk of developing type 2 diabetes.
The second type of PCOS is the post-pill type. This type of PCOS occurs after a woman stops taking birth control pills. It is characterized by irregular periods, acne, and increased hair growth. Women with this type of PCOS may also experience weight gain and difficulty losing weight.
The third type of PCOS is the inflammatory type. This type of PCOS is caused by inflammation in the body, and it is characterized by irregular periods, acne, and increased hair growth. Women with this type of PCOS may also experience fatigue, joint pain, and digestive issues.
The fourth type of PCOS is the adrenal type. This type of PCOS is caused by imbalances in the adrenal glands, which produce hormones such as cortisol and DHEA. Women with this type of PCOS may experience irregular periods, acne, and increased hair growth. They may also experience fatigue, anxiety, and depression.
It is essential to determine the subtype of PCOS a woman has to determine the best treatment plan. Treatment options for PCOS include lifestyle changes such as diet and exercise, medication, and surgery. Women with PCOS should work closely with their healthcare provider to develop a personalized treatment plan that addresses their unique needs.

Risk Factors and Causes of PCOS
Polycystic ovary syndrome (PCOS) is a complex endocrine disorder that affects women of reproductive age. The exact cause of PCOS is unknown, but it is believed to be a combination of genetic and environmental factors. In this section, we will discuss the various risk factors and causes of PCOS.
Genetics
Research has shown that PCOS tends to run in families, which suggests that genetics may play a role in the development of the condition. Women who have a mother or sister with PCOS are more likely to develop the condition themselves.
Hormonal Imbalance
PCOS is characterized by an imbalance of hormones, specifically an excess of androgens (male hormones) and insulin. This hormonal imbalance can lead to a variety of symptoms, including irregular menstrual cycles, acne, and hair growth on the face and body.
Insulin Resistance
Insulin resistance is a condition in which the body’s cells become less sensitive to insulin, which can lead to high blood sugar levels. Insulin resistance is common in women with PCOS, and it is believed to be a contributing factor to the development of the condition.
Obesity
Obesity is a common risk factor for PCOS, and it can exacerbate the symptoms of the condition. Women who are overweight or obese are more likely to experience irregular menstrual cycles, insulin resistance, and high levels of androgens.
Other Risk Factors
Other risk factors for PCOS include:
- Prediabetes or glucose intolerance
- High blood pressure
- Cholesterol abnormalities
- Sleep apnea
- Depression and anxiety
- Stress
- Thinning hair or hair loss
- Cardiovascular disease
- Stroke
- Gestational diabetes
As we’ve seen, PCOS is a complex condition with a variety of risk factors and causes. While the exact cause of PCOS is unknown, it is believed to be a combination of genetic and environmental factors. Understanding the risk factors and causes of PCOS is an important step in managing the condition and improving menstrual health.
Managing PCOS and Improving Menstrual Health
When it comes to managing PCOS and improving menstrual health, there are several options available to us. These options range from lifestyle changes to medications and hormonal birth control. Below, we’ll discuss some of the most effective ways to manage PCOS and improve menstrual health.
Lifestyle Changes
One of the most effective ways to manage PCOS and improve menstrual health is through lifestyle changes. This includes maintaining a healthy diet, engaging in regular physical activity, and managing inflammation. A healthy diet should include plenty of nutrient-dense foods such as fruits, vegetables, lean protein, and healthy fats. It’s also important to avoid processed foods, sugary drinks, and foods high in saturated and trans fats.
Regular physical activity can also help improve menstrual health by reducing inflammation, improving insulin sensitivity, and promoting weight loss. Aim for at least 150 minutes of moderate-intensity exercise per week, such as brisk walking, cycling, or swimming.
Managing inflammation is also important for improving menstrual health. This can be achieved by avoiding inflammatory foods such as processed meats, refined carbohydrates, and sugary drinks. Instead, focus on anti-inflammatory foods such as fatty fish, nuts, seeds, and leafy greens.
Medications
In some cases, medications may be necessary to manage PCOS and improve menstrual health. Medications such as metformin can help improve insulin sensitivity and regulate menstrual cycles. Hormonal medications such as birth control pills can also help regulate menstrual cycles and reduce symptoms such as acne and excess hair growth.
Hormonal Birth Control
Hormonal birth control can be an effective way to manage PCOS and improve menstrual health. Birth control pills can help regulate menstrual cycles and reduce symptoms such as acne and excess hair growth. Other forms of hormonal birth control, such as the patch or the ring, can also be effective.
Nutrients
Certain nutrients can also help manage PCOS and improve menstrual health. For example, magnesium can help reduce inflammation and improve insulin sensitivity. Zinc can help regulate menstrual cycles and reduce acne. Omega-3 fatty acids can also help reduce inflammation and improve menstrual health.
Quality of Life
Finally, it’s important to focus on improving our overall quality of life when managing PCOS and improving menstrual health. This includes getting enough sleep, managing stress, and engaging in activities we enjoy. By taking care of our overall health and well-being, we can improve our menstrual health and manage PCOS more effectively.
Overall, managing PCOS and improving menstrual health requires a multifaceted approach. By making lifestyle changes, taking medications if necessary, using hormonal birth control, focusing on nutrients, and improving our overall quality of life, we can effectively manage PCOS and improve menstrual health.